Diabetic Foot Ulcers: Essentials for Nurses
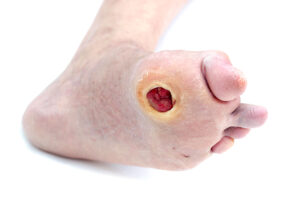
Diabetic foot ulcers pose a major threat to patients with diabetes. For instance, they often result in infections, amputations, and reduced mobility if left unmanaged. However, as nurses, your expertise in early detection, prevention, and education is vital. This guide covers the essentials and care strategies for diabetic foot ulcers. In this guide, we discuss assessment, treatment, and prevention tips. Integrate them into your practice for the best patient outcomes. With these basic principles, you’ll help mitigate risks and promote healing in this high-prevalence condition.
Understanding Diabetic Foot Ulcers
Diabetic foot ulcers typically arise from neuropathy, poor circulation, and impaired immune responses. As a result, minor injuries evolve into chronic ulcers. Common types include neuropathic ulcers on pressure points like the ball of the foot or toes. Meanwhile, ischemic ulcers stem from vascular issues. Additionally, neuroischemic hybrids blend both elements. These wounds heal slowly due to hyperglycemia. For example, it disrupts collagen synthesis and boosts infection susceptibility. Recognize the Wagner grading system. It spans from superficial (Grade 1) to deep tissue involvement with osteomyelitis (Grade 3+). Thus, nurses can classify severity and plan interventions promptly.
Identifying Risk Factors
Key risk factors heighten the likelihood. These encompass peripheral neuropathy, which causes loss of sensation. Peripheral artery disease cuts blood flow. Foot deformities like hammertoes or Charcot arthropathy generate pressure spots. Furthermore, poor glycemic control, smoking, obesity, and ill-fitting shoes contribute to calluses or blisters. Nurses should screen high-risk patients annually. Utilize tools like monofilament testing for neuropathy. Alternatively, apply ankle-brachial index for vascular status. Consequently, this identifies vulnerabilities early and prevents ulcer formation.
Prevention Strategies for At-Risk Feet
Prevention focuses on daily foot inspections for cuts or redness. Combine it with proper hygiene. Maintain moisturized skin without soaking to avoid maceration. Encourage protective footwear with cushioned insoles. Advise against barefoot walking, even indoors. Moreover, promote smoking cessation and balanced nutrition. Incorporate vitamins for tissue repair. Tight blood sugar management strengthens healing potential. Routine podiatry referrals manage nail care and callus removal. These measures help protect against trauma and prevent complications.
Comprehensive Wound Assessment
Thorough assessment starts with visual and palpation exams. Evaluate wound size, depth, exudate, odor, and surrounding tissue. Search for signs like warmth or swelling that indicate infection. Probe gently for undermining or bone exposure. Document using standardized scales for consistency. Assess sensation with a 10g monofilament. Employ Doppler for pulses if needed. Additionally, monitor systemic symptoms like fever. Infections can escalate rapidly in diabetics. For this reason, it’s important to take action quickly if you notice any signs of infection.
Effective Treatment Approaches
Treatment emphasizes offloading pressure. Debride to eliminate necrotic tissue. Select moisture-balanced dressings like hydrofibers for moderate exudate. Or choose alginates for heavier drainage. Antimicrobial options, such as silver-infused dressings, help fight infections. Advanced therapies like negative pressure wound therapy can assist with stubborn ulcers. Collaborate with the team and patient on glycemic optimization. Administer antibiotics if osteomyelitis is suspected. Always customize plans to wound stage and patient tolerance. This will ensure optimal recovery based on individual needs.
The Importance of Offloading and Footwear
Offloading redistributes weight from ulcer sites. Employ total contact casts, removable walkers, or therapeutic shoes. Custom orthotics tackle deformities. Educate on shoe fit with wide toe boxes and seamless interiors. This helps prevent recurrence. Compliance remains essential. Educate your patients and engage them in the decision process. Make sure to monitor for skin irritation from devices. When implemented consistently, offloading can significantly help with healing of diabetic foot ulcers.
Patient Education and Self-Management
Empower patients through tailored education. Concentrate on daily foot checks, proper nail trimming, and recognizing warning signs. These involve persistent redness or numbness. Utilize visual aids and simple language. Address hygiene, diet, and exercise impacts. Reinforce the connection between blood sugar control and wound healing. Involve family caregivers for support. Supply resources for ongoing monitoring. Simple steps like this promotes independence and cuts down on emergency visits.
Knowing When to Refer or Escalate Care
Refer promptly to specialists. For example, podiatrists can help to manage debridement. Vascular surgeons can handle poor perfusion. Infectious disease experts oversee resistant infections. Escalate if wounds deteriorate despite treatment. Watch for bone exposure or systemic illness. Multidisciplinary teams are essential to improve outcomes. Lastly, make sure your patient follows up to ensure continuity in complex diabetic foot cases.
Conclusion: Empowering Nurses in Diabetic Foot Care
Master these essentials to prevent, assess, and treat diabetic foot ulcers effectively. Consequently, you’ll preserve limbs and boost patient well-being. Remain vigilant and collaborative. This addresses this challenging aspect of diabetes management with confidence.
Ready to take your wound care expertise to the next level? Enroll in our upcoming Wound Care Certification Course (WCC Prep) at AppleTree CEU—designed for nurses like you to master advanced techniques and earn your certification. Available now! Enroll Here
